» Treatment Guidelines

What is Cornelia de Lange Syndrome
Cornelia de Lange Syndrome (CdLS) is a rare developmental disorder that is present from birth. The syndrome was named after the Dutch children’s doctor Cornelia de Lange, who first described the disorder in 1933 (1). It is estimated that between 1 in 10,000 and 1 in 30,000 people in the population have CdLS (2).
CdLS can affect many parts of the body and individuals with CdLS may display physical, cognitive and behavioural characteristics (1). Cognitive characteristics are brain-based processes like memory and thinking. Behavioural characteristics refer to certain behaviours that individuals with CdLS are more likely to have. These characteristics can vary widely among affected individuals and range from small differences compared to other people to very noticeable differences.
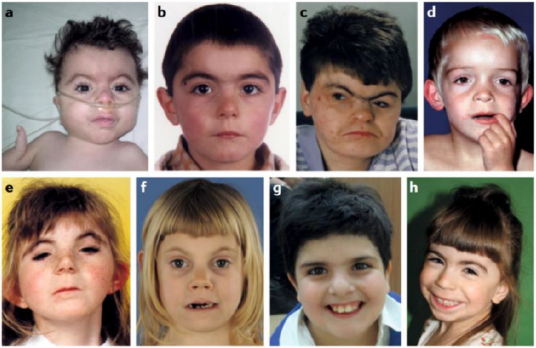
Classic (or typical) CdLS can be easily recognised from birth by an experienced children’s doctor (paediatrician) or clinical geneticist (a doctor who diagnoses and supports families with genetic disorders). This is because individuals with CdLS often have distinctive facial features, growth patterns, and limb differences (see Figure 1 on the next page). These characteristics form the classic CdLS phenotype, which the physical, cognitive and behavioural characteristics associated with the syndrome.
It is important to note that if a person has a diagnosis of CdLS it does not mean they will display all the characteristics associated with the syndrome. There may be different degrees of difference in the face and limbs for example. It is also very important to remember that everyone with CdLS is an individual and will also have characteristics passed down from their family.
CdLS is a genetic disorder. This means that it is caused by a change in genetic material; this change is called a mutation. The genetic causes of CdLS are complicated and research to fully understand all the genetic causes is still ongoing. CdLS is usually caused by a change in one of seven genes (individual genetic instructions in DNA that make us who we are). The seven genes associated with CdLS are named: NIPBL, SMC1A, SMC3, RAD21, BRD4, HDAC8 and ANKRD11. A change in one of these genes affects the ‘cohesin complex’. This means that the cohesin protein complex does not function as it should in the cells of the body, causing altered human development. See the section ‘What causes Cornelia de Lange Syndrome’ on page 7 for more information.
|
Fig. 1 | Facial phenotype of individuals with Cornelia de Lange Syndrome. a | Classic Cornelia de Lange Syndrome (CdLS) phenotype resulting from an NIPBL variant. b | Non-classic CdLS phenotype in an individual with an NIPBL variant. c | Adult with NIPBL variant and classic phenotype. d | Non-classic phenotype in individual with an SMC1A variant. e | Classic phenotype in an individual with an SMC3 variant. f | Non-classic phenotype in an individual with a RAD21 variant. g | Non-classic phenotype in an individual with an HDAC8 variant. h | Non-classic phenotype in an individual with an ANKRD11 variant. |
For example, some changes in the SMC1A gene have been identified in individuals with characteristics that resemble Rett syndrome (another neurodevelopmental disorder associated with intellectual disability) and few characteristics that resemble CdLS. This is despite SMC1A being confirmed as a causal gene for CdLS (3). Another example is that some individuals have changes in genes (such as ANKRD11 and NAA10) that are associated with developmental disorders other than CdLS but they show characteristics associated with the CdLS phenotype (4,5).
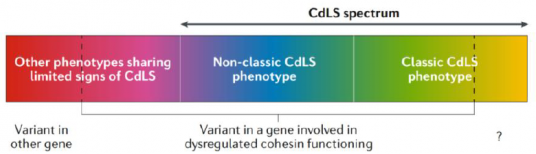
As a result, the overall CdLS phenotype has been characterised as a spectrum, implying a range of clinical findings and characteristics (see Figure 2, page 4). The CdLS spectrum includes the classic (typical) CdLS phenotype, alongside other syndromes with similar but non-classic (atypical) characteristics of CdLS, which are caused by changes in genes associated with CdLS.
Note: Syndromes caused by changes in genes associated with CdLS, but without many CdLS characteristics are not included in the spectrum.
|
Fig. 2 | The phenotypes classified as Cornelia de Lange Syndrome (CdLS) can be defined as a spectrum. All seven identified genes that are associated with CdLS affect the cohesin complex (explained further on page 7). The CdLS spectrum includes individuals with the classic CdLS phenotype in whom the affected gene has or has not been identified (if a genetic test is unable to identify a CdLS diagnosis, this can be determined through assessment of clinical features). The spectrum also includes individuals with a non-classic CdLS phenotype who have a gene variant affecting the cohesin complex. There are also individuals who carry a gene variant involved in cohesin functioning (see page 7) but present little or no resemblance to the classic CdLS phenotype. These individuals do not fall within the CdLS spectrum. Note that both classic and non-classic CdLS may affect individuals mildly or severely. The question mark in the figure indicates that there may be genes causing CdLS spectrum that do not have a cohesin function; such genes are unknown at present, but they may exist and must not be excluded. |
Grouping individuals affected into the CdLS spectrum helps knowledge exchange and contact between affected individuals and their families. This means individuals and families can support each other; and leads to increased attention from researchers. However, identification of differences between individuals within the CdLS spectrum is also important to tailor care to each individual.
The International CdLS Consensus Group
Due to the great variability of the CdLS spectrum, as well as in the care and management of individuals, a group of international experts have formed the “International CdLS Consensus Group” to make a series of recommendations. Experts in this group are part of the Scientific Advisory Council of the World Federation of CdLS Support Groups. These recommendations are outlined and explained throughout this document and the full list of recommendations is also available at the end.
|
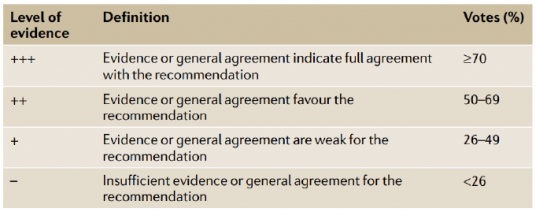
Table 1 | Details of the Delphi consensus voting process (structured communication process between a panel of experts used to gain consensus on the CdLS recommendations).
37 international experts voted on the recommendations digitally. For all recommendations, over 90% of experts were in full agreement with the recommendations. Patient group representatives did not vote. |